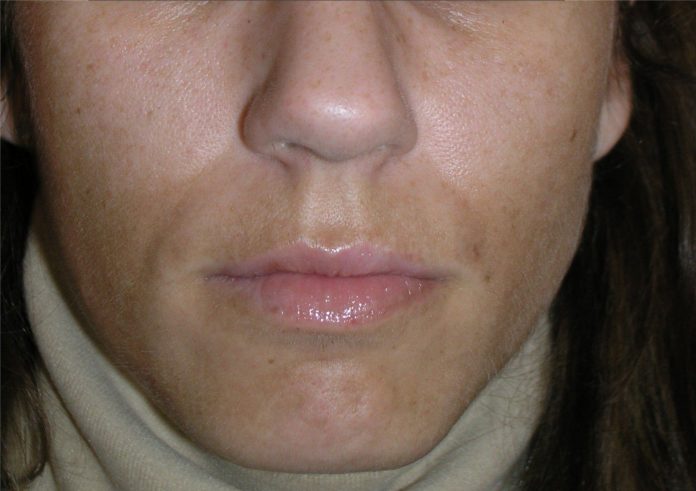
What is the ‘mask of pregnancy’ and what does it look like?
The ‘mask of pregnancy’, also known as Melasma or Chloasma (medical names) is a skin condition that occurs in 45-75% of pregnancies. The name originates from the Greek word melas, which means black. In this condition, areas of the face become darkened (hyperpigmented). The darkened areas generally appear as blotchy, irregular shaped patches on the face that may range from tan to dark brown in colour.
It is not an infection, it is not contagious and it is not due to an allergy. Also, it is not cancerous and will not change into skin cancer.
There is variation in how the mask of pregnancy appears between individuals. In some women, the darkened patch (lesions) may be lighter, while in others it will be darker. Some women may just have one lesion, while other women may have multiple lesions.
The location in which darkening occurs may also vary. Usually, it will fall into one of three main patterns:
- Centrofacial pattern – this is the most common type occurring in 63% of those affected. The darkening typically occurs in central areas of the face and can be widespread including the forehead, upper lip, nose, chin and cheeks.
- Malar pattern – seen in 21% of affected women. In this case, the darkening only affects the cheeks and nose.
- Mandibular pattern – is the least common pattern occurring in 16% of affected women. In this type, the darkening is only found on the skin overlying the outermost part of the jaw bone (ramus).
Who is most susceptible?
 Women with dark hair, brown eyes and dark complexions are more likely to be affected. Therefore it is more common in Latin/Hispanic, North African, African-American, Asian, Indian, Middle Eastern, and Mediterranean populations. It is also more commonly seen in those who have had an affected blood relative. It is also more common in women of Hispanic origin.
Women with dark hair, brown eyes and dark complexions are more likely to be affected. Therefore it is more common in Latin/Hispanic, North African, African-American, Asian, Indian, Middle Eastern, and Mediterranean populations. It is also more commonly seen in those who have had an affected blood relative. It is also more common in women of Hispanic origin.
Why does the mask of pregnancy occur?
The skin changes that occur are the result of increased numbers of the pigment producing cells in the skin (melanocytes). No one really knows exactly what causes the increased numbers of these cells to occur, but most agree that it is related to the increased levels of hormones in pregnancy. These include:
- Melanocyte stimulating hormone – a hormone that stimulates melanocytes – the cells in the body that produce pigment and give rise to darker skin, freckles, birthmarks (naevi) etc.;
- Oestrogen; and
- Progesterone.
Some also believe that there are substances from the placenta that may cause changes at a genetic level.
Regardless of the underlying cause, exposure to UV light has been consistently shown to be a major factor leading to the development of these skin changes.
Other causes include:
- Medications – some women notice similar changes when taking the oral contraceptive pill or hormone replacement treatment. arsenic, metals such as silver, gold and copper as well as some medications used to prevent seizures;
- Older cosmetics with poorly refined ingredients can irritate the face and sensitise it to these changes;
- Nutrition;
- Liver disease;
- Thyroid dysfunction including hypo- or hyper-thyroidism;
- Endocrine disorders such as Addison’s disease;
- Familial factors – it is particularly common in women with Hispanic origins and women with dark hair, dark skin and brown eyes; and
- Some parasitic infections.
When does the mask of pregnancy occur?
Onset is generally in the second and third trimesters of pregnancy.
The majority of cases tend to occur in the warmer months when there is usually increased sun exposure.
How long does the mask of pregnancy last?
Depending on the individual, the skin changes may continue to progress during the pregnancy. The mask of pregnancy almost always resolves following delivery of the baby, with most women finding that their skin has gone back to normal by their baby’s first birthday. In only 10% of women do the skin changes persist.
How is the mask of pregnancy treated?
 The mask of pregnancy will generally fade over time following the delivery of your baby.
The mask of pregnancy will generally fade over time following the delivery of your baby.
You can take preventative measures and prevent further progression of the condition by:
- Minimising your sun exposure and avoid sunbathing / sun tanning – Avoid outdoors when the UV index is high (between 10am and 3pm). Generally only 30mins of exposure to the neck hands and arms when the UV index is low is sufficient for adequate vitamin D synthesis – you can discuss this with your General Practitioner as it will vary depending on your skin type, individual risk factors, location and season of the year.
- Use sunscreen on sun exposed areas; with a sun protection factor (SPF) of 30 or greater and a high ultraviolet A (UVA) star-rating. Ideally this should be applied at least 20 minutes before going outside.
- Wear appropriate clothing / sun protection.
- Avoid cosmetics that irritate your skin and those with additives such as perfumes.
There are multiple creams/lotions that can be used to help reduce the skin changes. These are typically prescribed by doctors who specialise in the treatment of skin conditions (called dermatologists). Treatment is usually only used in those women in which the mask of pregnancy does not resolve itself following delivery of the baby. Treatment is not recommended during pregnancy for several reasons:
- The hormones that are the cause of the skin condition persist during pregnancy, and hence it is harder to treat;
- Most cases resolve on their own once the baby is born, although this may take some months; and
- The treatments used can be harmful to the developing baby.
During your pregnancy or after the birth of your baby, you can consider camouflaging the skin changes with cosmetics. Foundations and powders with a white or yellow undertone can minimise the appearance.
If it hasn’t resolved by baby’s 1st birthday, you can speak with a dermatologist about:
- Facial creams such as hydroquinone, tretinoin and/or fluocinolone acetonide
- Facial chemical peels
- Dermabrasion
- Laser therapy
Kindly written and reviewed by Dr Allison Johns BSc (Hons) MBBS, Doctor, King Edward Memorial Hospital and Editorial Advisory Board Member of Parenthub and Virtual Medical Centre.
References
- Ingber, A. Obstetric Dermatology: A practical guide. 2009. Springer-Verlag, Berlin Heidelberg.
- Black, M (ed). Obstetric and Gynaecologic Dermatology. 3rd Edition. 2008. Elsevier, China.
- Melasma. The British Association of Dermatologists (cited 28 September 2012). Available from (URL)
- Melasma: who gets and causes. American Academy of Dermatology. Online (cited 28 September 2012). Available from: (URL)
- Schalock PC, Isu JTS, Arndt KA (eds). Lippincott’s Primary Care Dermatology. 2010. Lippincott Williams & Wilkins.
- Stalgis-Bilinski KL, Boyages J, Salisbury EL, Dunstan CR, Henderson SI, Talbot PL. Burning daylight: balancing vitamin D requirements with sensible sun exposure 2011; 194:345-348. (Full text)
- Melasma: tips for managing. American Academy of Dermatology. Online (cited 28 September 2012). Available from: (URL)



 (6 votes, average: 4.17 out of 5)
(6 votes, average: 4.17 out of 5)