University of Sydney experts say a causal relationship between Zika virus infection during pregnancy and microcephaly is strongly suspected but not yet proven as the WHO declared the mosquito-borne virus a global public health threat.
The World Health Organisation Director-General Margaret Chan has declared the outbreak of Zika virus a public health emergency – only the fourth time the WHO has declared a state of emergency.
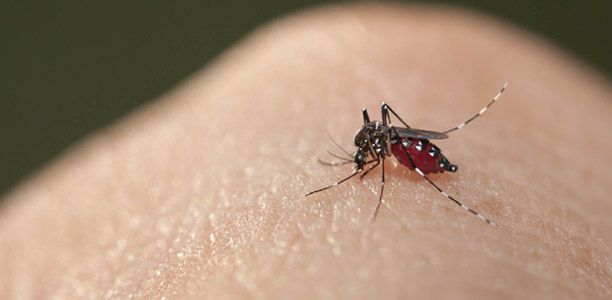
It’s estimated there are more than four million people living in areas populated by the Yellow Fever mosquito (Aedes aegypti), which is responsible for spreading the disease.
Yellow fever mosquito, which is present in far north Queensland, can also spread dengue fever, chikungunya, yellow fever viruses and other diseases.
The Pan American Health Organisation says that Zika has spread in 24 nations and territories in the Americas, with reports it is rife in Asia.
“Declaring Zika virus a public health emergency has happened relatively early in the outbreak compared to the comparable declaration for Ebola virus,” says Dr Grant Hill-Cawthorne, a medical virologist from the University of Sydney.
Addressing a media conference today, he said the WHO declaration reflects a need by the global community to deal with infectious disease emergencies more rapidly.
“We need to communicate the risks to these people. We need the global community to get on board to aid in control efforts in South America and the other areas affected by the Zika virus.”
The virus is suspected of causing thousand of birth defects in Brazil but no firm causal link has been established. The first reported case of Zika infection was in 1947 in a macaque in Ziika forest, Uganda, after which the virus is also named.
“The emergency alert is a call to arms to focus on research in this area, particularly to establish a clear link between the Zika virus and the reported subsequent birth defects, especially microcephaly, which refers to reduced head size and brain damage,” he said.
Pregnant women travelling to countries with the Zika virus should apply insect repellents containing DEET or picaridin early in the morning, said University of Sydney entomologist, Dr Cameron Webb.
While echoing a federal government warning to reconsider travelling to 22 nations where Zika is transmitted, Dr Webb acknowledged it might be impossible for everyone to avoid or delay their travel plans.
Explaining how transmission of the virus could occur in Australia, Dr Webb said: “What happens is someone steps off the plane, shortly after they arrive in Australia they’re bitten by a local yellow fever mosquito who becomes infected and can pass the virus on to the local community.
“In the absence of the yellow fever mosquito in our major cities, the risk of outbreak are low,” he said. “We do have these mosquitoes in far north Queensland, areas around Cairns and Townsville are the places where we might likely get a small outbreak of Zika virus.”
Dr Webb said that if the virus were to spread to far north Queensland, Australian authorities would be well prepared. The yellow fever mosquito posed a threat to people because it had migrated out of the jungle and into the cities, but it could not survive in the southern states as the winters were too cold, he noted.
“Because 80% of infections are asymptomatic there’s quite a significant likelihood of infected people returning to Australia, but unless they happen to travel to far north Queensland, the risk of them being bitten by an appropriate mosquito is relatively small,” said the University of Sydney’s Professor Lyn Gilbert, who is clinical lead of Infection Prevention and Control at the Western Sydney Local Health Network.
Dr Grant Hill-Cawthorne says it’s likely the Australian Government will be asked to contribute to a global effort led by the WHO against Zika. “A lot of the efforts will now be on countries like Australia to help South American countries to get on top of this.
“I think it would be very prudent, particularly considering that we are likely to see cases in Northern Queensland, it would be in Australia’s best interest to try and help on the ground where the concentration of cases are greatest.”
(Source: The University of Sydney)