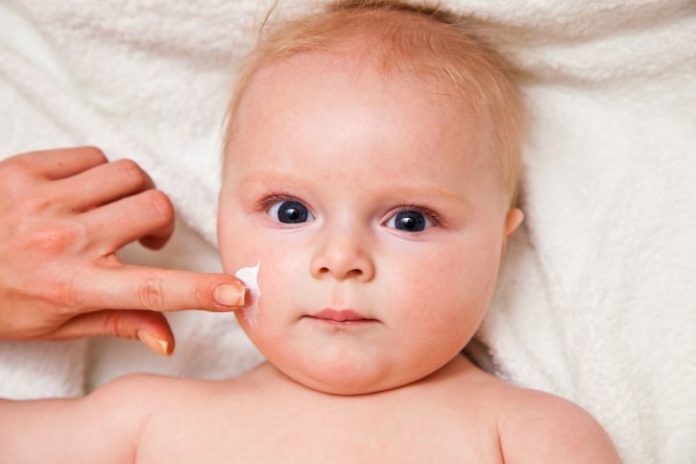
Parents are either too scared of the medications to treat a common childhood skin rash or too relaxed about them, says leading dermatologist.
“It was really upsetting to find my beautiful baby had developed this rash all over her body,” admits Roberta Hourn, mother of eczema sufferer Kali, who is now 9 years old. “I thought it was my fault but soon realized what it was. But when the doctor said she wanted to use steroids on it, I was very nervous. I’d heard horror stories of skin damage.”
“Australian children have amongst the highest rates of eczema in the world – and up to one in three children may develop eczema” says dermatologist Ann Maree Kurzydlo. Given it’s such a common condition, it’s important for parents to know there are effective ways of managing eczema and treating it. It’s also important to understand there is no cure for eczema, and control is the aim of treatment. However, we often see parents both over and under-treating eczema.
“In terms of prevention there is a lot that can be done. Occasionally there’s a food allergy but the main thing is that children with eczema have dry skin and if you keep it moist by restoring the skin barrier, you minimise itching and flares. I recommend short warm baths or showers and the use of a soap and fragrance- free products. A good moisturiser needs to be applied liberally following the bath or shower and reapplied once or twice a day. Parents often use small amounts of moisturiser, when liberal application is what’s needed.
“These general measures should be a daily routine, and there is additional treatment needed when the eczema flares. We use topically applied steroids as a mainstay of treatment. These are cortisone-based products. Some parents have what we call steroid phobia.
They’re often concerned about side effects, particularly thinning or damaging the skin. In fact, an Australian study found that if used correctly as directed by a dermatologist or GP, these sorts of issues are very uncommon. At the other end of the spectrum we find parents using steroid cream when it’s not really needed. The trouble with overuse is the effects of the steroids on the eczema wear off.
So when there is a flare, and we need to get on top of it, the steroid creams or ointments are less effective. The technical term for this is tachyphylaxis.”
“When it was explained to me that if you use the right steroids at the right time – in other words when the eczema is active, we can nip it in the bud and then go back to relying on moisturisers as a daily routine,” says Roberta Hourn, “I got the hang of it and relaxed. Mind you it took some getting used to, slapping on the large amounts of moisturizer cream that were needed.”
“The message here is that parents need to keep steroid ointments in reserve for when the eczema flares” says Dr Kurzydlo. “this allows us to achieve more rapid and effective control. On the other hand, general skin care measures including use of a moisturiser, should be a daily routine.”
The Eczema Association of Australasia raised this issue of steroid use for eczema treatment as a public health initiative during Eczema Awareness Week – 3 – 9 September 2012.
“We urge parents to consult their GP or Dermatologist and discuss this issue,” said Cheryl Talent, President of the Eczema Association of Australasia.
“Used properly steroids can greatly relieve eczema suffering at appropriate times and more information about this issue can be obtained on our educational website at www.eczema.org.au or by calling (cost of a local call) 1300 300 182.
What is eczema?
Atopic dermatitis, or eczema, is a common, recurring, non-infectious, inflammatory skin disease in which the skin becomes red, dry, itchy or scaly and may weep, bleed and crust over. Eczema belongs to the category of diseases called ‘atopic’, a term often used to describe allergic conditions for which there is usually a family history. The ‘atopic triad’ of allergies comprises eczema, asthma and hayfever, with many sufferers experiencing all three conditions. Severe eczema can significantly impact on a child’s quality of life and social development. The word ‘eczema’ comes from the Greek word meaning “to boil over”.
It is the incessant itch of eczema that separates it from other skin diseases such as psoriasis. Eczema can spread over the entire body, but commonly affects the face, hands and creases of the elbows and knees. Triggers of eczema can include soaps, bubble baths and other toiletries, dust mites, pollens, grass, sand, animal dander, woollen and synthetic fabrics, chemicals, preservatives, fragrances, extreme changes in temperature, food and stress. Increasingly evidence suggests patients with eczema have an underlying impaired skin barrier.
A change of seasons can trigger an eczema ‘flare up’. Research has shown more than half of people with eczema believe that their flares are worse in winter to early spring, which is usually related to skin dryness.
The common symptoms of eczema include:
- Dry skin
- Inflammation – redness & swelling of the skin
- Intense itching (pruritus)
- Scratch marks
- Thick, dry, leathery skin
- Small, raised blister-like bumps that may open when scratched, which weep and crust and may become infected.
 Prevalence
Prevalence
Australia has one of the highest incidences of eczema world-wide. Eczema affects up to one in three Australians at some time during their life. The skin disease is most prevalent in children, with up to 90 per cent of cases developing symptoms by age five. However eczema can occur in people of any age.
The prevalence of eczema has increased two-to-three fold in recent years. Research shows the increase is linked to a range of environmental factors. Around 60 per cent of people with eczema will develop symptoms within the first 12 months of life. While some of these people will outgrow symptoms, others will have the skin disease for life.
Family history
Although eczema is thought to be hereditary, around 30 per cent of people affected by the skin disease do not have a family history of allergic diseases. A child with both parents who have an atopic condition, such as eczema, asthma or hayfever, has an 80 per cent chance of inheriting eczema.
Treatment
A person with eczema can spend up to $2000 or more every year managing their disease. 40 per cent of people with eczema use four or more products to treat their eczema. Managing eczema to prevent flares is a constant battle involving daily moisturising with emollients, avoidance of allergens and irritants, dietary restrictions, using flare prevention products at the first signs of redness and itch, plus the application of topical steroid creams should a severe flare occur.
The skin is the largest organ in the body. The regular use of moisturisers assists in reducing the rate of water loss through the skin and maintaining a protective barrier against infection.
Impact
The relentless itching and scratching of eczema can lead to sleep disturbance, infections, days off work and school, social isolation and loss of self-esteem. Eczema may also have a major impact on daily life. Those affected by eczema should avoid contact with triggers and allergens. Common activities that can cause discomfort to eczema sufferers or aggravate the condition include swimming, gardening and exercise.
Source: Eczema Association of Australia



 (6 votes, average: 4.33 out of 5)
(6 votes, average: 4.33 out of 5)